Abstract
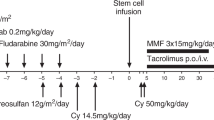
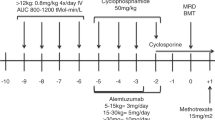
Myeloablative HLA-matched related donor (MRD) hematopoietic stem cell transplantation (HSCT) is a potentially curative treatment for children with sickle cell disease (SCD), achieving survival rates over 90%. However, optimal conditioning for older SCD patients undergoing MRD transplantation is unknown. We evaluated a novel conditioning regimen comprising thymoglobulin, thiotepa, cyclophosphamide, fludarabine, and total-body irradiation (200 cGy). Graft-versus-host disease (GVHD) prophylaxis included post-transplant cyclophosphamide (100 mg/kg), mycophenolate mofetil, and sirolimus. We aimed to improve donor engraftment rates, decrease GVHD, and minimize toxicity. A total of 25 patients were prospectively recruited in a multicentre study across three sites; 22/25 (88%) were fully matched, and 3/25 (12%) received a one-antigen-mismatched sibling transplant. 12% (3/25) of patients had experienced a second graft failure from a previous HCT. 11 participants (44%) received bone marrow, while 14 (56%) received peripheral blood as stem cell sources. The median age was 26.7 years (IQR, 18.53–32.02), and the median follow-up was 42 months (IQR, 30-49). The estimated 5-year event-free survival rate was 96%, and the 2-year overall survival rate was 100%. No graft failure was observed. Median whole blood chimerism at day +28 and day +365 engraftment was 100% and 97%, respectively. Among evaluable participants, 17/21 (81%) were off immunosuppression at 1-year post-transplant. The 1-year grade III-IV acute GVHD rate was 4% (n = 1), with no chronic GVHD. This regimen produced high engraftment and survival in this cohort using our novel conditioning regimen for MRD HSCT in adolescents and adults with severe SCD, including those undergoing a second HSCT. Optimal donor engraftment is associated with a lower risk of secondary myeloid neoplasms.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Piel FB, Steinberg MH, Rees DC. Sickle Cell Disease.2017; 376: 1561-73. https://doi.org/10.1056/NEJMra1510865.
Bernaudin F, Socie G, Kuentz M, Chevret S, Duval M, Bertrand Y, et al. Long-term results of related myeloablative stem-cell transplantation to cure sickle cell disease. Blood. 2007;110:2749–56.
Gluckman E, Cappelli B, Bernaudin F, Labopin M, Volt F, Carreras J, et al. Sickle cell disease: an international survey of results of HLA-identical sibling hematopoietic stem cell transplantation. Blood. 2017;129:1548–56.
Chaturvedi S, Ghafuri DL, Jordan N, Kassim A, Rodeghier M, DeBaun MR. Clustering of end-organ disease and earlier mortality in adults with sickle cell disease: A retrospective-prospective cohort study. Am J Hematol. 2018;93:1153–60.
Gladwin MT, Sachdev V, Jison ML, Shizukuda Y, Plehn JF, Minter K, et al. Pulmonary hypertension as a risk factor for death in patients with sickle cell disease. N Engl J Med. 2004;350:886–95.
Kassim AA, Payne AB, Rodeghier M, Macklin EA, Strunk RC, DeBaun MR. Low forced expiratory volume is associated with earlier death in sickle cell anemia. Blood. 2015;126:1544–50.
McClellan AC, Luthi JC, Lynch JR, Soucie JM, Kulkarni R, Guasch A, et al. High one year mortality in adults with sickle cell disease and end-stage renal disease. Br J Haematol. 2012;159:360–7.
Platt OS, Brambilla DJ, Rosse WF, Milner PF, Castro O, Steinberg MH, et al. Mortality in sickle cell disease. Life expectancy and risk factors for early death. N Engl J Med. 1994;330:1639–44.
Eapen M, Brazauskas R, Walters MC, Bernaudin F, Bo-Subait K, Fitzhugh CD, et al. Effect of donor type and conditioning regimen intensity on allogeneic transplantation outcomes in patients with sickle cell disease: a retrospective multicentre, cohort study. Lancet Haematol. 2019;6:e585–96.
Hsieh MM, Fitzhugh CD, Weitzel RP, Link ME, Coles WA, Zhao X, et al. Nonmyeloablative HLA-matched sibling allogeneic hematopoietic stem cell transplantation for severe sickle cell phenotype. JAMA. 2014;312:48–56
Alzahrani M, Damlaj M, Jeffries N, Alahmari B, Singh A, Rondelli D, et al. Non-myeloablative human leukocyte antigen-matched related donor transplantation in sickle cell disease: outcomes from three independent centres. Br J Haematol. 2021;192:761–8.
Guilcher GMT, Truong TH, Saraf SL, Joseph JJ, Rondelli D, Hsieh MM. Curative therapies: Allogeneic hematopoietic cell transplantation from matched related donors using myeloablative, reduced intensity, and nonmyeloablative conditioning in sickle cell disease. Semin Hematol. 2018;55:87–93.
Saraf SL, Oh AL, Patel PR, Jalundhwala Y, Sweiss K, Koshy M, et al. Nonmyeloablative Stem Cell Transplantation with Alemtuzumab/Low-Dose Irradiation to Cure and Improve the Quality of Life of Adults with Sickle Cell Disease. Biol Blood Marrow Transplant. 2016;22:441–8.
Kassim AA, de la Fuente J, Nur E, Wilkerson KL, Alahmari AD, Seber A, et al. An international learning collaborative phase 2 trial for haploidentical bone marrow transplant in sickle cell disease. Blood. 2024;143:2654–65.
Wood JC. Guidelines for quantifying iron overload. Hematology Am Soc Hematol Educ Program. 2014;2014:210–5.
Eapen M, Brazauskas R, Williams DA, St Walters MC, Martin A, Jacobs BL, et al. Secondary Neoplasms After Hematopoietic Cell Transplant for Sickle Cell Disease. J Clin Oncol. 2023;41:2227–37.
Lawal RA, Mukherjee D, Limerick EM, Coles W, Hsieh MM, Dillon LW, et al. Increased incidence of hematologic malignancies in SCD after HCT in adults with graft failure and mixed chimerism. Blood. 2022;140:2514–18.
Jacobs JW, Adkins BD, Stephens LD, Woo JS, Booth GS. Risks and benefits of cannabis as a pain control modality in patients with sickle cell disease. Clin Hematol Int. 2023;5:47–50.
Popham E, Moeller K, Raj A. Effects of Erythrocytapheresis Procedures on Delayed Bone Marrow Conversion in Sickle Cell Disease. Clin Hematol Int. 2022;4:144–7.
Bolanos-Meade J, Hamadani M, Wu J, Al Malki MM, Martens MJ, Runaas L, et al. Post-Transplantation Cyclophosphamide-Based Graft-versus-Host Disease Prophylaxis. N Engl J Med. 2023;388:2338–48.
Oostenbrink LVE, Pool ES, Jol-van der Zijde CM, Jansen-Hoogendijk AM, Vervat C, van Halteren AGS, et al. Successful mismatched hematopoietic stem cell transplantation for pediatric hemoglobinopathy by using ATG and post-transplant cyclophosphamide. Bone Marrow Transplant. 2021;56:2203–11.
Kean LS, Burns LJ, Kou TD, Kapikian R, Lozenski K, Langston A, et al. Abatacept for acute graft-versus-host disease prophylaxis after unrelated donor hematopoietic cell transplantation. Blood. 2024;144:1834–45.
Patel DA, Dhedin N, Chen H, Karnik L, Gatwood K, Culos K, et al. Early viral reactivation despite excellent immune reconstitution following haploidentical Bone marrow transplant with post-transplant cytoxan for sickle cell disease. Transpl Infect Dis. 2020;22:e13222.
Wachsmuth LP, Patterson MT, Eckhaus MA, Venzon DJ, Gress RE, Kanakry CG. Post-transplantation cyclophosphamide prevents graft-versus-host disease by inducing alloreactive T cell dysfunction and suppression. J Clin Invest. 2019;129:2357–73.
Marty FM, Ljungman P, Chemaly RF, Maertens J, Dadwal SS, Duarte RF, et al. Letermovir Prophylaxis for Cytomegalovirus in Hematopoietic-Cell Transplantation. N Engl J Med. 2017;377:2433–44.
Passweg JR, Baldomero H, Atlija M, Kleovoulou I, Witaszek A, Alexander T, et al. The 2023 EBMT report on hematopoietic cell transplantation and cellular therapies. Increased use of allogeneic HCT for myeloid malignancies and of CAR-T at the expense of autologous HCT. Bone Marrow Transplant. 2025;60:519–28.
Acknowledgements
The work was supported by the 3 participant institutions, KFSHRC, VUMC & KAMC.
Author information
Authors and Affiliations
Contributions
RA, AA and AK wrote the initial draft of the manuscript, RA, AA, FM, MA, AK enrolled and cared for participants, and reviewed the paper; JF, AP, KW edited the manuscript, TA completed the statistical analysis.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alasbali, R., Alzahrani, M., Wilkerson, K. et al. Excellent outcomes using a novel reduced intensity conditioning with thiotepa and post-transplant cyclophosphamide for HLA-matched related donor transplant in adolescents and adults with sickle cell disease. Bone Marrow Transplant (2026). https://doi.org/10.1038/s41409-026-02876-3
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41409-026-02876-3